The end-to-end automation layer for modern 340B programs
Plenful’s 340B Audit & Optimization Suite fully automates a 100% audit of eligible 340B claims, uncovers missed savings and intelligently streamlines the referral capture process.
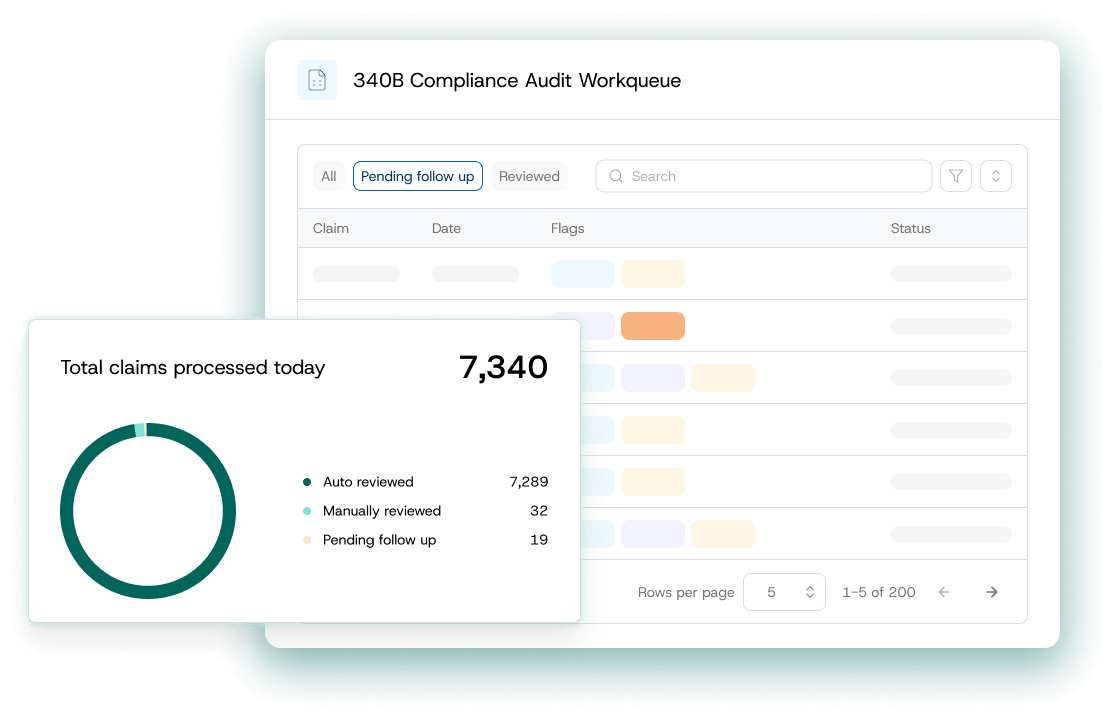

.png)






.png)






.png)






.png)






Covered Entities face intense pressure to manage regulatory complexity and protect 340B savings
Compliance Exposure & Program Vulnerability
Manual audit processes make it nearly impossible for 340B programs to scale. Teams are often limited to spot audits—leaving thousands of claims unchecked and exposing programs to compliance risk. Misclassified claims, inconsistent data, and messy audit trails only compound the problem. Without a centralized platform to track, search, and validate claims activity, teams remain anxious about audit readiness and the potential for findings that could jeopardize their program eligibility.
Missed Savings from Fragmented Workflows
Siloed data and rigid eligibility logic create blind spots that hide millions in potential 340B savings. Referral data is often scattered across disparate systems, making it a “needle in a haystack” to find eligible claims. The result: missed opportunities, inefficiencies, and a lack of clear visibility into program performance. Most Covered Entities don’t have the bandwidth or analytics infrastructure to uncover these insights—let alone act on them.
Changing Legislation & Program Requirements
New and evolving policies—like the 340B Rebate Model Pilot and Medicare Drug Price Negotiation Program—are reshaping the 340B landscape. These changes will require teams to rapidly adapt operational processes, reporting structures, and financial oversight models. The organizations that succeed will be those that modernize early—using automation to stay compliant, nimble, and financially resilient amid growing regulatory complexity.
Streamline your compliance efforts. Maximize savings recapture. Sleep at night.
Built for 340B teams, Plenful’s 340B Audit & Optimization suite centralizes your disparate claims data, automates claim-level logic, and delivers actionable insights—turning hours of manual review into minutes of intelligent validation.
Strengthen Compliance Posture
Validate 100% of eligible 340B claims against HRSA requirements and your Covered Entity’s Policies & Procedures through automated verification. Plenful works across owned, contract, and mixed-use settings.
Recapture Missed 340B Savings
Pinpoint high-value claims that should qualify for 340B pricing but were incorrectly classified as ineligible, recapturing lost revenue quickly and confidently.
Referral Capture & Network Transparency
Automate referral pathway verification with provider matching and documentation tracking across your network to uncover additional savings recovery from referral-based prescriptions.
Executive 360 Dashboards & Insights
Plenful brings fragmented claims data into a single, summarized view. Track KPIs, monitor program performance, and demonstrate measurable ROI from one executive dashboard.

For Operators, By Operators
"Utilizing Plenful helps me sleep at night, knowing our 340B program is compliant. With Plenful, we're now auditing 100% of our 340B claims."
Thomas Kim



.png)


