Four Key Challenges to Prepare for as Medicare’s Maximum Fair Price Takes Effect
Medicare’s Maximum Fair Price (MFP) officially went live on January 1st. Select Medicare Part D drugs are now subject to negotiated pricing under the Inflation Reduction Act, with 15 additional Part D drugs set to come online in 2027 and beyond.
We’re partnering with a number of large health systems as a Third-Party Support Entity (TPSE), receiving access to MTF remittance information on behalf of pharmacies through the MTF, as well as claims and 340B eligibility data via pharmacy management systems and TPAs. This has given our team a front row seat to the complex MFP refund reconciliation efforts required, and where the greatest financial risks have been identified.
On average, we’re identifying up to 20% of MFP refunds as missing.
This reality is building urgency for those pharmacy or finance teams who have not developed a MFP strategy.
MFP is more than a simple pricing adjustment. It introduces a new reconciliation workflow, unique cash-flow dynamics, and complexity that pharmacy teams will need to actively manage.
Read on for a summary of what we’re hearing from Plenful customers partnering with Plenful to reconcile their refunds, and how our MFP Management solution is adding value.
MFP is live, but reconciliation strategies are still forming
MFP applies to a limited set of Part D drugs, but its footprint will expand quickly. That matters because the program’s design places a meaningful share of the operational complexity downstream.
Under MFP, pharmacies dispense and adjudicate Part D prescription claims as they do today. Reimbursement from Part D plan sponsors for the select MFP drugs is now limited to the Maximum Fair Price (MFP) plus a dispensing fee. Plans submit prescription claim information to CMS’s Drug Data Processing System (DDPS), which then passes specific data elements along to the Medicare Transaction Facilitator (MTF) Data Module (DM). Manufacturers utilize the claims data from the MTF DM to determine which claims are eligible for an MFP refund and the appropriate amount, a process called “Effectuation”. Manufacturers have 14 days to effectuate the refund and return the corresponding data to the MTF DM.
Given the various stakeholders and the number of steps involved, pharmacies may wait to see their refunds up to 28 days from the prescription claim’s adjudication.
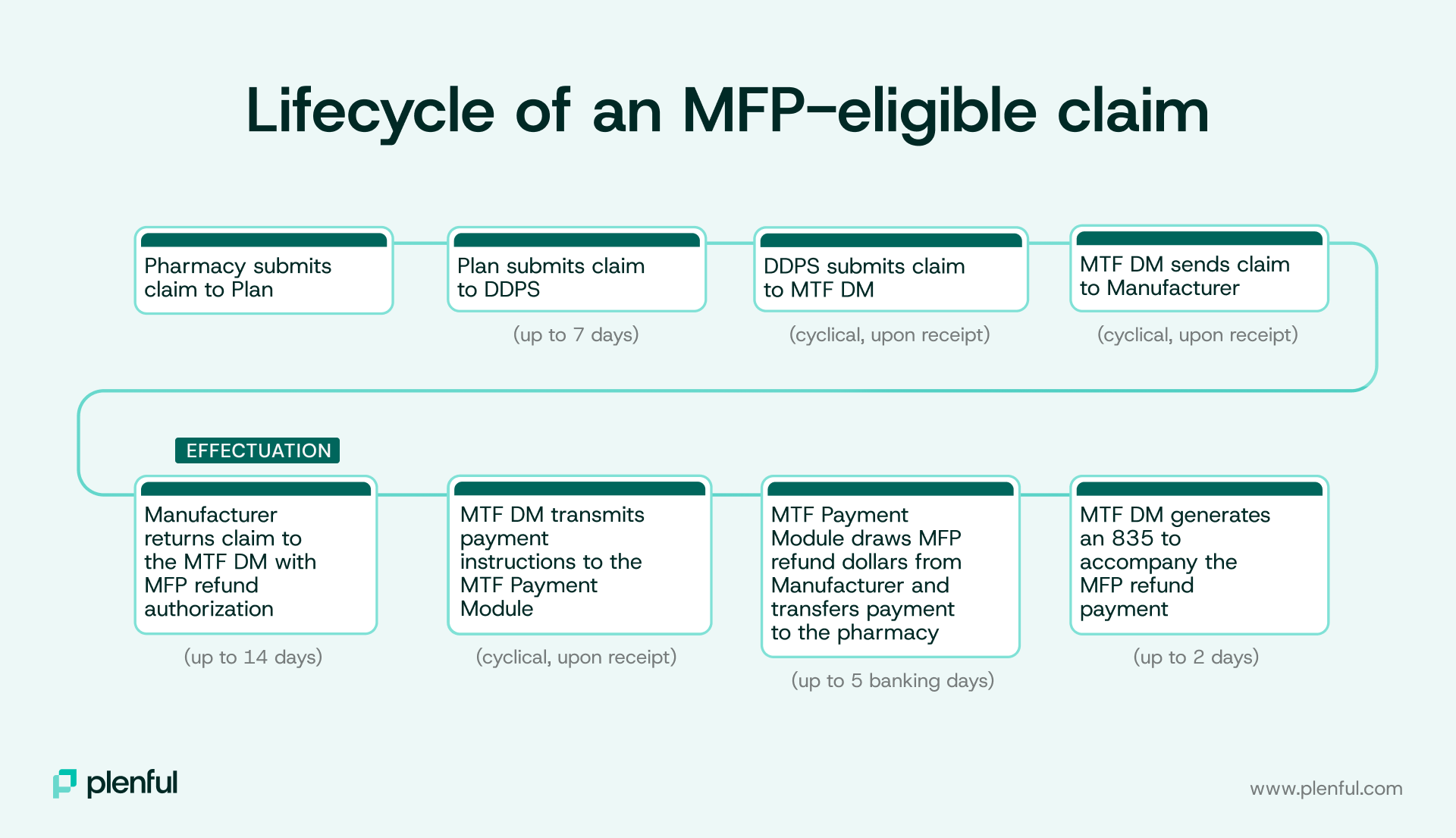
As a result, many covered entities are working hard to improve financial oversight and their reconciliation process. Here’s what the complexity of MFP can mean for pharmacies of covered entities, and four key challenges to consider:
Challenge 1: Missing MFP refunds
The first challenge is to ensure your pharmacies are not missing MFP refunds. Manufacturers must rely on limited and imperfect signals, such as modifiers, self-identification, or evidence of purchasing patterns, to determine 340B eligibility.
Manufacturers have already publicly flagged (see pg. 5) this limitation: they do not have complete visibility into 340B eligibility based on available data shared from covered entities. Only covered entities possess definitive 340B determination data.
Consequently, during the effectuation process, if a manufacturer mistakenly assumes a claim is 340B—and the 340B price is lower than the MFP price—no MFP refund will be issued.
Challenge 2: MFP–340B duplication creates structural complexity
Identifying and resolving duplication between MFP and 340B pricing is another challenge. When both programs apply to the same claim, the lower price will always prevail.
In practice, if a 340B claim receives an MFP refund, de-duplication occurs on the MFP side. If MFP is below the 340B price, the pharmacy will still receive an MFP refund; however, it will be less than normal because the refund will be calculated as MFP minus 340B acquisition price. If the 340B price is below the MFP, the MFP would be credited to the pharmacy to be utilized on a future MFP-eligible claim.
This de-duplication process creates real financial complexity. Because credits are applied to future claims, the financial trail becomes harder to follow over time.
Challenge 3: Duplication credits are difficult to track manually
The third challenge is the crediting model itself.
Tracking these credits across pharmacies, claims, and manufacturers is manageable in theory, but extremely difficult in practice without the right tools.
For pharmacy teams already stretched thin, manually reconciling credits requires maintaining detailed claim history and understanding when and how credits are applied. If an error occurs, the burden falls on the pharmacy to identify the issue and initiate a correction. Manufacturers will accept feedback and attempt to address corrections via processes like Good Faith Inquiry Forms (see pg. 6), now managed via Beacon for dispute resolution, but this requires time, effort, and oversight from already lean teams.
As more drugs are added to MFP, this will become increasingly complex. Without clear visibility, it becomes harder to answer a basic question finance teams care deeply about: Were we actually made whole?
Challenge 4: Reconciliation volume creates a capacity problem
Unlike the proposed 340B Rebate Program Pilot, MFP is not a data submission problem. Pharmacies are not submitting claim files. Instead, the complexity shows up after the fact, during MFP refund reconciliation.
Each MFP-eligible Part D claim must be reviewed to confirm:
- Whether MFP was applied during drug acquisition or retrospectively via refund
- Whether the expected refund was received
- Whether any credits were issued or applied
- Whether the purchase acquisition price changed the refund calculation
For pharmacies with meaningful Part D volume in MFP drugs, this quickly becomes a claim-by-claim exercise. That creates a capacity issue, not just an administrative one. Teams must invest time and attention simply to build confidence in their revenue timing and cash flow—work that grows as the program expands.
Why automated financial reconciliation is critical as MFP scales
As MFP expands to more drugs and thus more claim volume, it will become increasingly difficult for pharmacies to manage reconciliation through manual workflows alone. The combination of missing refunds, ledger-based credits, and 340B de-duplication creates a new level of operational complexity that didn’t exist previously.
At Plenful, we’ve built a solution to support covered entities participating in MFP, drawing on the same principles that have guided our work in 340B Rebate Management.
Our MFP Reconciliation Management solution
As a designated Third-party Support Entity (TPSE), our solution automates reconciliation and increases visibility around new MFP refunds to reduce the administrative burden on pharmacies.
Plenful's MFP Management solution will:
- Access MTF data and remittance information on behalf of pharmacies through the MTF as a Third Party Support Entity (TPSE)
- Reconcile expected vs. received MFP refunds at the claim level
- Identify duplications or credits in scenarios where both MFP and 340B apply
- Provide clear, claim-level visibility and reporting within Executive 360 Dashboards so pharmacy leaders can confidently manage revenue timing and cash flow, and feel prepared to report key learnings
The goal is not just efficiency, but giving both pharmacy and finance teams a confident and reliable way to understand where money is owed, where it has been paid, and where follow-up is required.
See what we’ve built for MFP Reconciliation Management
Pharmacy leaders who start paying attention now will be better positioned as the program expands. Understanding where refunds can go missing, manufacturer credit utilization, and where reconciliation breaks down is the first step toward building durable operations under MFP.
If you’d like to demo our MFP Reconciliation Management solution, please request time here to connect 1-1 with our sales team.
I'd also welcome connecting 1-1 with you on LinkedIn.
– Tim L’Hommedieu, PharmD, MS, and SVP of Pharmacy
Related blogs
.png)
Customer Story: Mercy Medical Center’s Modern 340B Lever

Pharmacy in 2035: Key Takeaways from Becker’s CPO Summit

Welcoming Dustin Eubanks as SVP of Strategic Partnerships



